Knee Recovery Milestone Tracker
Early Steps (Days 1-14)
Focus on icing to kill swelling and prevent joint stiffness. Avoid pushing too hard to prevent increased inflammatory response.
What to Watch For:
- Excessive swelling in the joint
- Inability to stand within 24 hours
- Severe post-operative pain
Key Recovery Milestones
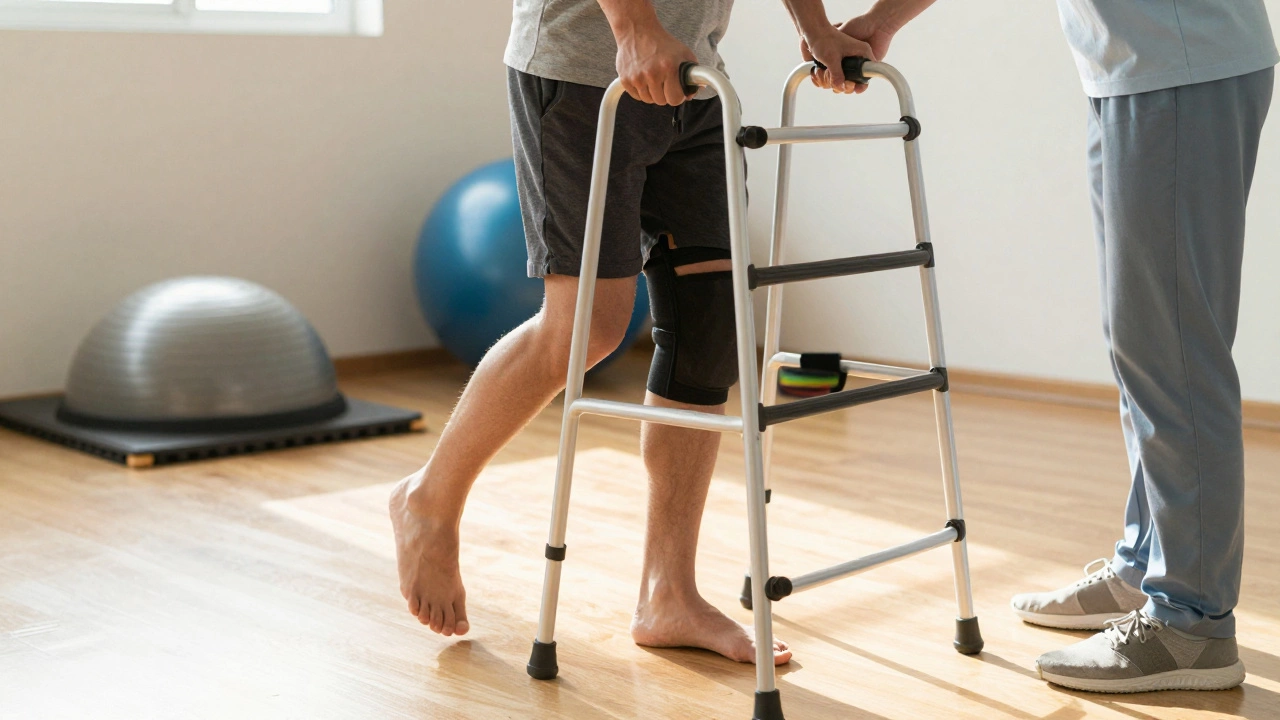
- Days 1-3: First steps with a walker or walker-assisted frame.
- Weeks 1-6: Transitioning from walkers to canes or independent walking.
- Months 3-6: Returning to "functional" walking (grocery shopping, short strolls).
- Months 6-12: Achieving a "normal" gait and full strength.
The First Few Steps: Day Zero to Week Two
The clock starts ticking the moment you leave the operating room. In modern orthopedics, the goal is "early mobilization." You won't be lounging in bed for a week. In fact, Total Knee Arthroplasty is a surgical procedure where a damaged knee joint is replaced with an artificial prosthesis made of metal and high-grade plastic. Because the goal is to prevent blood clots and stiffness, most surgeons want you standing within 24 hours.
During these first fourteen days, your "walk" won't look normal. You'll likely be using a walker to keep your weight off the joint while the surgical incision heals. You'll feel a lot of swelling, which is a natural part of the inflammatory response. The focus here isn't on speed or grace; it's about safely getting from the bed to the bathroom. You'll be dealing with Post-operative Pain, which is typically managed with a combination of nerve blocks and oral medications. If you push too hard here, you risk increasing swelling, which actually slows down your range of motion.
The Transition Phase: Weeks Three to Six
This is where the real work happens. By week three, many patients start feeling an itch to ditch the walker. Your surgeon might clear you to move to a cane or a walker with one wheel. This period is all about Physical Therapy, which is a specialized healthcare treatment using exercise and manual therapy to restore movement and strength to a joint. Without it, the new joint can stiffen up, leading to a permanent limp.
You'll start working on your "gait training." This is just a fancy way of saying you're relearning how to walk without leaning to one side. A common mistake people make is "guarding" the leg-walking with a bent knee to avoid pain. Your therapist will push you to fully straighten the leg (extension) and bend it (flexion). If you can't get your knee to 0 degrees (perfectly straight), you'll never walk normally because your leg will always feel like it's slightly buckled.
Regaining Functional Independence: Months Two to Four
By the second or third month, most people can walk around the house without any aids. You might find that you can go to the mailbox or walk through a store without thinking about every single step. However, "walking around the house" and "walking normally" are two different things. You might still have a slight hitch in your step, and your endurance will be low. You'll notice that walking for 20 minutes leaves you exhausted or makes the knee feel "hot."
This is the phase where Proprioception-your brain's ability to sense where your joint is in space-starts to return. Since you've likely spent years walking with a painful, arthritic knee, your brain has developed "bad habits." You have to consciously override those patterns. This is why balance exercises, like standing on one leg or using a foam pad, are critical during this window.
| Timeline | Walking Aid | Primary Goal | Common Sensation |
|---|---|---|---|
| Week 1-2 | Walker / Frame | Safe mobility | Tightness, swelling |
| Week 3-6 | Cane / Single Crutch | Range of motion | Soreness after PT |
| Month 2-3 | None (Short distances) | Normal gait pattern | Stiffness after rest |
| Month 6+ | None | Endurance & Speed | Near-normal feel |
The Final Stretch: Six Months to One Year
Many patients get frustrated around the six-month mark. They think, "I had surgery, why do I still feel a little stiff?" Here is the secret: internal healing takes much longer than the skin takes to close. The deeper tissues, the bone integration of the Prosthetic Implant, and the surrounding ligaments are still remodeling. It is very common to feel a "click" in the knee or some lingering swelling after a long day of walking.
True "normalcy" usually hits between nine and twelve months. This is when the muscle strength in your Quadriceps (the big muscle on the front of your thigh) finally catches up. Because the quads are the primary stabilizers of the knee, any weakness here will make your walk look unnatural. Once those muscles are strong enough to support your full body weight during the "push-off" phase of a step, the limp usually vanishes.
What Slows Down the Process?
Not everyone recovers at the same speed. A few things can throw a wrench in your timeline. First, your pre-surgery health. If you have Diabetes, your wound healing might be slower, which can delay your transition to unassisted walking. Second, your commitment to PT. There's a big difference between doing your exercises because the therapist told you to and doing them because you're determined to walk without a limp.
Another factor is the Surgical Approach used. For instance, a minimally invasive approach might lead to faster initial recovery, but the ultimate destination-walking normally-remains the same regardless of the technique. Finally, psychological factors play a role. Fear of falling or fear of "breaking" the new knee can lead to cautious, stiff movements that actually prolong the recovery of a natural gait.

Tips for Speeding Up Your Return to Normal Walking
If you want to get back to your natural stride faster, focus on these three things: icing, extension, and consistency. Icing isn't just for pain; it kills the swelling that prevents you from straightening your leg. If your knee is swollen, it's like trying to bend a hinge that has a pebble stuck in it. Get the swelling down, and the movement follows.
Focus heavily on "terminal knee extension." This means getting that last few degrees of straightness. Many people can bend their knee fine, but they can't get it perfectly flat. If you can't get it flat, you'll always walk with a slight crouch. Use a rolled-up towel under your ankle to let gravity pull the knee straight for 10 minutes a day.
Lastly, walk often, but in short bursts. Instead of trying to walk for 30 minutes once a day, walk for 5 minutes every hour. This prevents the joint from "freezing up" and teaches your brain that walking is a safe, normal activity again.
Will I ever walk exactly the same as before?
For the vast majority of patients, yes, and often better. Since the surgery removes the bone spurs and inflammation that caused you to limp in the first place, you can actually achieve a more symmetrical gait than you had before the surgery. However, it takes a year of muscle rebuilding to get there.
Is it normal to still have a limp after 3 months?
Yes, it is very common. This is usually due to a combination of residual swelling and muscle atrophy in the quadriceps. If you are consistently doing your physical therapy and your range of motion is improving, a slight limp at three months is not typically a cause for alarm.
When can I stop using a cane?
Most people transition away from a cane between week 4 and week 8. You should only stop using it when you can walk a short distance without leaning to one side and without experiencing a significant increase in pain. Your physical therapist will usually give you the "green light" based on your balance and strength.
Can I walk too much during recovery?
Yes. Overdoing it in the first two months can lead to excessive swelling, which actually hinders your range of motion. If you notice your knee is warmer than usual or the skin is tight and shiny, you've likely pushed too far. Balance activity with plenty of elevation and icing.
What if my knee feels like it's "clicking" while I walk?
Clicking or popping sounds are incredibly common after a knee replacement. This is usually just the prosthetic components interacting or air bubbles shifting in the joint fluid. As long as the clicking isn't accompanied by sharp pain or new instability, it's generally considered normal.
Next Steps and Troubleshooting
If you are further along in your recovery (6+ months) and still feel you aren't walking "normally," it's time to evaluate your muscle balance. Often, the calves are tight and the quads are weak. Adding a gentle stretching routine for the Achilles tendon and increasing the resistance in your leg presses can help.
For those struggling with balance, consider a low-impact activity like swimming or using an elliptical machine. These tools allow you to practice the walking motion without the full impact of your body weight, helping you refine your coordination before you hit the pavement.
If you experience a sudden return of pain, a fever, or a calf that is warm and swollen, contact your surgical team immediately. While most recovery issues are just about timing and effort, these can be signs of a blood clot or infection that requires immediate medical attention.