IVF Journey Interactive Roadmap
Click on each phase of the IVF process to learn what happens, how long it takes, and the primary goal of that stage.
Ovarian Stimulation
Doctors use hormones like FSH to encourage the ovaries to produce multiple eggs instead of the usual one. This involves several weeks of injections to maximize the chances of success.
Imagine the frustration of doing everything right-tracking cycles, eating clean, reducing stress-and still seeing a negative pregnancy test. For many, the biological machinery just isn't clicking. That's where IVF treatment is a medical process where an egg is fertilized by sperm outside the body, in a laboratory setting, before being transferred into the uterus. It isn't just a "last resort" anymore; it's a precise science that bypasses blocked tubes or low sperm counts to give people a real shot at parenthood.
Quick Summary: The IVF Essentials
- Core Purpose: Fertilizes eggs in a lab to bypass reproductive barriers.
- Success Factors: Age, egg quality, and the skill of the embryologist.
- Typical Timeline: Usually takes about 4 to 6 weeks per cycle.
- Main Goal: To achieve a healthy pregnancy by selecting the strongest embryo.
What actually happens during the IVF process?
If you've ever wondered if IVF is just a fancy version of natural conception, think of it as a controlled shortcut. In a natural pregnancy, the egg and sperm meet in the fallopian tube. IVF moves that entire meeting to a petri dish. This allows doctors to see exactly what's happening and intervene if things aren't moving along.
The process starts with Ovarian Stimulation. In a normal month, a woman typically releases one egg. To increase the odds of success, doctors use hormones like FSH (Follicle Stimulating Hormone) to encourage the ovaries to produce multiple eggs. You'll likely spend two weeks taking injections in your abdomen. It's a bit nerve-wracking at first, but most people get the hang of it quickly.
Once the eggs reach the right size, a "trigger shot" is given to time the final maturation. Then comes the Egg Retrieval. This is a minor surgical procedure where a doctor uses an ultrasound-guided needle to gently collect the eggs from the follicles. You're usually under light sedation, so you won't feel a thing during the 20-minute process.
The Lab Work: Where the Magic Happens
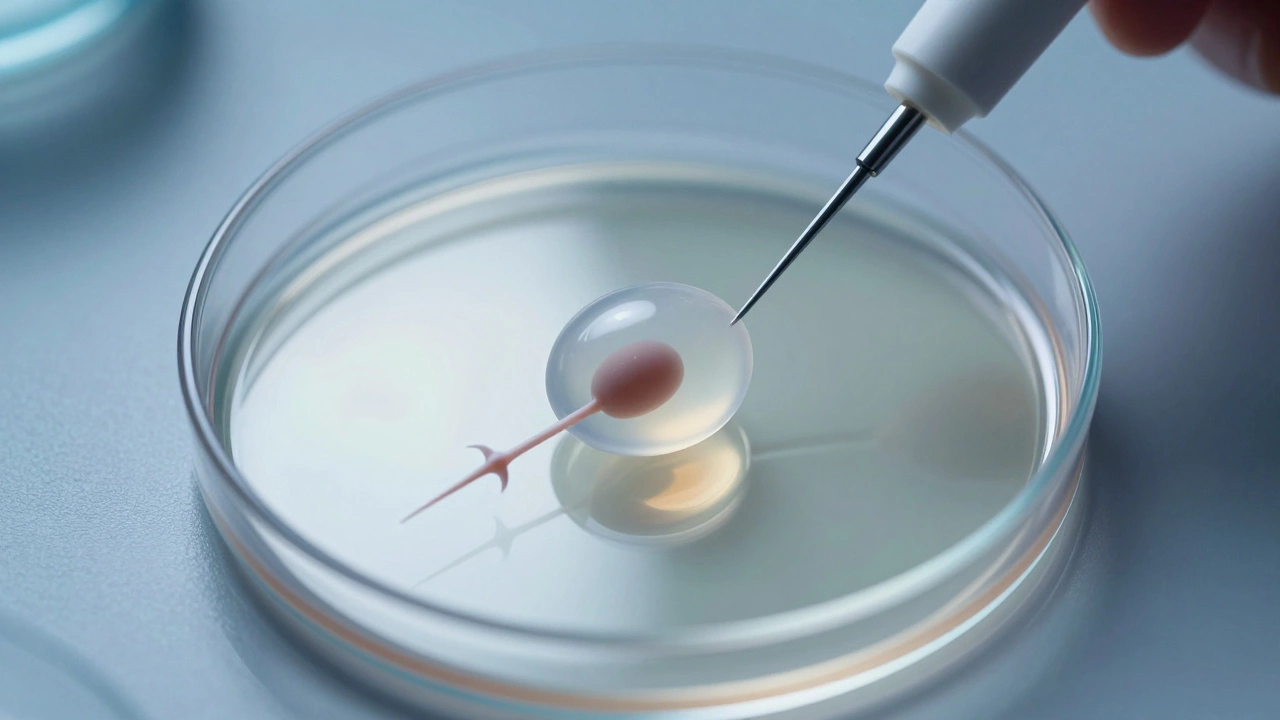
While the eggs are being collected, the partner provides a sperm sample, or the clinic uses donor sperm. The Embryologist then steps in. Depending on the situation, they use one of two methods: standard fertilization or ICSI (Intracytoplasmic Sperm Injection). With ICSI, a single, healthy sperm is injected directly into the egg. This is a game-changer for couples dealing with severe male infertility.
Over the next few days, the lab monitors the eggs. If fertilization works, they grow into embryos. Most clinics let the embryos grow for 3 to 5 days until they reach the Blastocyst stage. This is the point where the embryo is most likely to implant successfully in the womb.
| Feature | Natural Conception | IVF Treatment |
|---|---|---|
| Location of Fertilization | Fallopian Tube | Laboratory Dish |
| Egg Quantity | Usually 1 per cycle | Multiple (Stimulated) |
| Control over Sperm/Egg | None | High (Screening/ICSI) |
| Bypasses Blocked Tubes? | No | Yes |
The Final Step: Embryo Transfer
Once a high-quality embryo is selected, it's time for the Embryo Transfer. The doctor uses a thin catheter to place the embryo directly into the uterus. There's no anesthesia for this; it feels similar to a pap smear. Then, you wait. The "two-week wait" is often the hardest part of the whole journey, as you anticipate whether the embryo will implant.
Some people opt for a Frozen Embryo Transfer (FET). This happens when embryos are frozen (cryopreserved) and transferred at a later date. This is often safer because it allows the woman's body to recover from the hormone-heavy stimulation phase, potentially improving the uterine lining for a better chance of pregnancy.
Who actually needs IVF?
It's not just for people who have been trying for years. Some conditions make IVF treatment the most logical path from the start. For example, if someone has Endometriosis that has scarred the fallopian tubes, the egg simply can't reach the sperm. IVF skips the tubes entirely.
It's also the primary solution for PCOS (Polycystic Ovary Syndrome) when other medications fail to induce ovulation. Additionally, for LGBTQ+ couples or single parents, IVF provides the necessary framework to use donor gametes and achieve a biological connection to their child.
Genetic screening is another huge advantage. Using PGT (Preimplantation Genetic Testing), doctors can check embryos for chromosomal abnormalities or specific genetic diseases before they are transferred. This significantly reduces the risk of miscarriage and ensures the baby is healthy.
What are the risks and side effects?
No medical procedure is without a catch. The most common issue is OHSS (Ovarian Hyperstimulation Syndrome). This happens when the ovaries overreact to the fertility drugs, causing bloating, nausea, and in rare cases, fluid buildup in the abdomen. Most clinics prevent this by "freezing all" embryos and delaying the transfer until the body settles.
There is also the emotional toll. The cycle of hope and disappointment can be draining. It's not uncommon for the first round to fail. Success rates depend heavily on the woman's age-women under 35 have much higher success rates than those over 40, as egg quality naturally declines.
As for multiple births, IVF does increase the chance of twins or triplets if multiple embryos are transferred. However, the modern trend is "Single Embryo Transfer" (SET) to ensure a safer pregnancy for both the mother and the baby.

Pro Tips for Your IVF Journey
- Prepare your lining: Focus on a balanced diet and moderate exercise before starting your cycle to ensure your uterus is receptive.
- Ask about the lab: Not all labs are equal. Ask about their "fertilization rate" and the technology they use for incubation.
- Mental health first: Find a support group or a therapist who specializes in infertility. The hormones can make you emotional; you'll need a vent system.
- Plan your finances: IVF can be expensive. Check if your insurance covers any part of the process or if the clinic offers payment plans.
Is IVF painful?
The hormone injections can cause some bruising and soreness at the injection site. The egg retrieval is done under sedation, so you won't feel pain during the procedure, though you might feel some cramping afterward. The embryo transfer is generally painless and similar to a pelvic exam.
What is the success rate of IVF?
Success varies wildly based on age. For women under 35, success rates per cycle can be 50% or higher. For women over 40, the rate drops significantly, often below 20% when using their own eggs. This is why donor eggs are a common alternative for older patients.
How long does one IVF cycle take?
A typical cycle lasts about 4 to 6 weeks. This includes the stimulation phase (about 10-14 days), the retrieval, the lab growth period (3-5 days), and the final transfer. If you choose to freeze the embryos, the transfer can happen months later.
Can I do IVF if I have low sperm count?
Yes, absolutely. In cases of low sperm count or motility, doctors use ICSI (Intracytoplasmic Sperm Injection). This allows them to pick the single best sperm and inject it directly into the egg, bypassing the need for the sperm to swim on its own.
What happens to unused embryos?
Unused embryos are usually cryopreserved (frozen) for future use if the first attempt fails or if the parents want more children. If they are no longer needed, parents can choose to donate them to other couples, donate them to science, or have them discarded.
Next Steps and Troubleshooting
If you're just starting out, your first stop should be a fertility specialist for a baseline check-up. This usually involves blood tests to check your hormone levels (like AMH for ovarian reserve) and an ultrasound to look at your follicles.
If your first IVF cycle fails, don't panic. It doesn't mean it'll never work. Doctors often analyze the first cycle to adjust the medication dosage or change the timing of the trigger shot. Some people find that switching to a frozen transfer (FET) improves their results because it removes the stress of the stimulation drugs from the implantation window.
For those who experience repeated implantation failure, ask your doctor about an endometrial biopsy or a hysteroscopy. Sometimes the issue isn't the embryo, but the environment of the uterus, which can often be treated with medication or a simple surgical procedure.