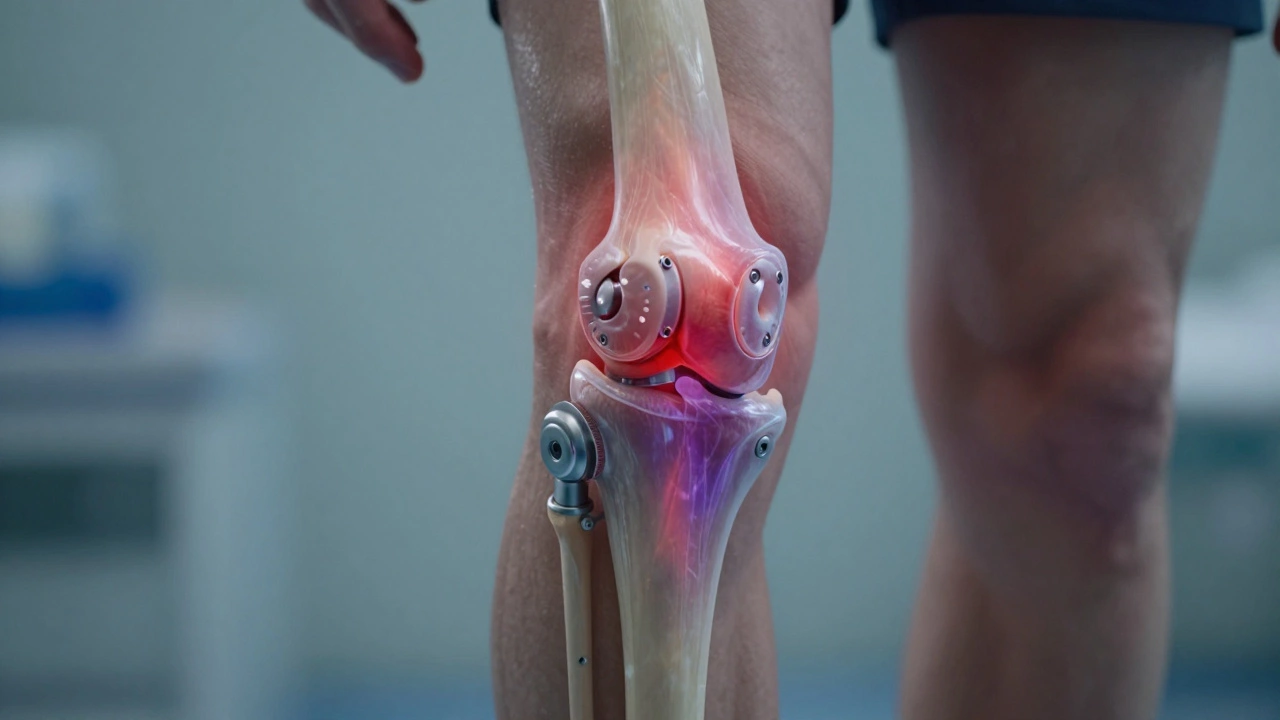
Post-Op Knee Pain Symptom Checker
Enter your details and select symptoms to receive personalized guidance based on standard recovery protocols.
Select "Warning Signs" only if you suspect a complication.Recommended Actions:
Most people think the worst part of knee replacement surgery is the moment the surgeon cuts into your leg. They are wrong. The sharp sting of the incision fades quickly thanks to modern anesthesia and nerve blocks. The real challenge begins hours later, when the drugs wear off and you realize that moving your new joint feels like trying to bend a rusted hinge.
If you are preparing for this procedure or currently sitting in the recovery room wondering why it hurts so much, you need to understand what kind of pain is normal, what causes it, and how to manage it without relying solely on heavy medication. Knowing what to expect helps you stay calm and focused on recovery.
The First 48 Hours: The Peak of Discomfort
The first two days after surgery are usually the hardest. This isn't just about the cut; it's about the inflammation your body creates as a natural response to trauma. During the operation, the surgeon removes damaged bone and cartilage and attaches metal and plastic components to your femur and tibia. This process irritates the surrounding tissues, muscles, and nerves.
You will likely have an spinal block or epidural during the surgery. This numbs your leg completely for several hours. When this numbness wears off, you might feel a sudden rush of sensation. It can be shocking. The pain often feels deep and throbbing rather than sharp. Many patients describe it as a heavy, swollen ache that radiates up the thigh and down the calf.
- Throbbing: Caused by blood flow returning to the limb and initial swelling.
- Burning: Often related to nerve irritation near the incision site.
- Stiffness: Your muscles tighten up to protect the injured area, making movement difficult.
This phase requires strict adherence to your pain management plan. Don't wait until the pain becomes severe to take your medication. Staying ahead of the pain allows you to move sooner, which actually reduces long-term discomfort.
Muscle Soreness vs. Surgical Pain
A common source of confusion is distinguishing between pain from the incision and pain from muscle fatigue. During a total knee arthroplasty (TKA), the surgeon must detach certain tendons and ligaments to access the joint. Specifically, the quadriceps tendon is often manipulated. These muscles haven't worked properly in months due to arthritis, so they are weak. Suddenly asking them to stabilize your leg again causes significant soreness.
This muscle pain typically peaks around day three or four. By then, the acute surgical pain has subsided somewhat, but your legs feel like you ran a marathon. You might experience cramping in the calves or tightness in the front of the thigh. This is not a sign that something is wrong; it is a sign that your body is healing and adapting to the new mechanics of your knee.
To mitigate this, gentle massage above the knee (not directly on the incision) and proper hydration help flush out metabolic waste products from the muscles. Heat packs can also relieve muscle tension, but always check with your surgeon before applying heat to ensure the wound is closed enough to prevent infection.
Why Bending the Knee Hurts So Much
One specific movement stands out as particularly painful: bending the knee. In the early stages, achieving even 90 degrees of flexion can feel like hitting a wall. This resistance comes from two sources: swelling inside the joint capsule and scar tissue formation.
When you bend your knee, you compress the tissues behind the joint. If there is fluid buildup (effusion), this compression increases pressure significantly. Additionally, your brain interprets the unfamiliar sensation of the new implant as a threat, causing reflexive muscle guarding. Your quadriceps lock up to prevent you from bending further, creating a cycle of stiffness and pain.
| Pain Type | Likely Cause | Typical Duration | Management Strategy |
|---|---|---|---|
| Sharp Incisional Pain | Skin and tissue cutting | 1-2 weeks | Painkillers, keeping wound dry |
| Deep Throbbing | Inflammation and bone remodeling | 3-5 days | Elevation, ice, NSAIDs |
| Muscle Cramping | Quadriceps and hamstring fatigue | 2-4 weeks | Gentle stretching, hydration |
| Stiffness/Burning | Nerve regeneration and scar tissue | Several months | Physical therapy, desensitization |
Physical therapy starts almost immediately. The therapist will guide you through passive range-of-motion exercises where they move your leg for you. This bypasses the muscle guard and helps stretch the joint capsule gently. Consistency here is key. Skipping sessions leads to increased stiffness, which makes future movements more painful.
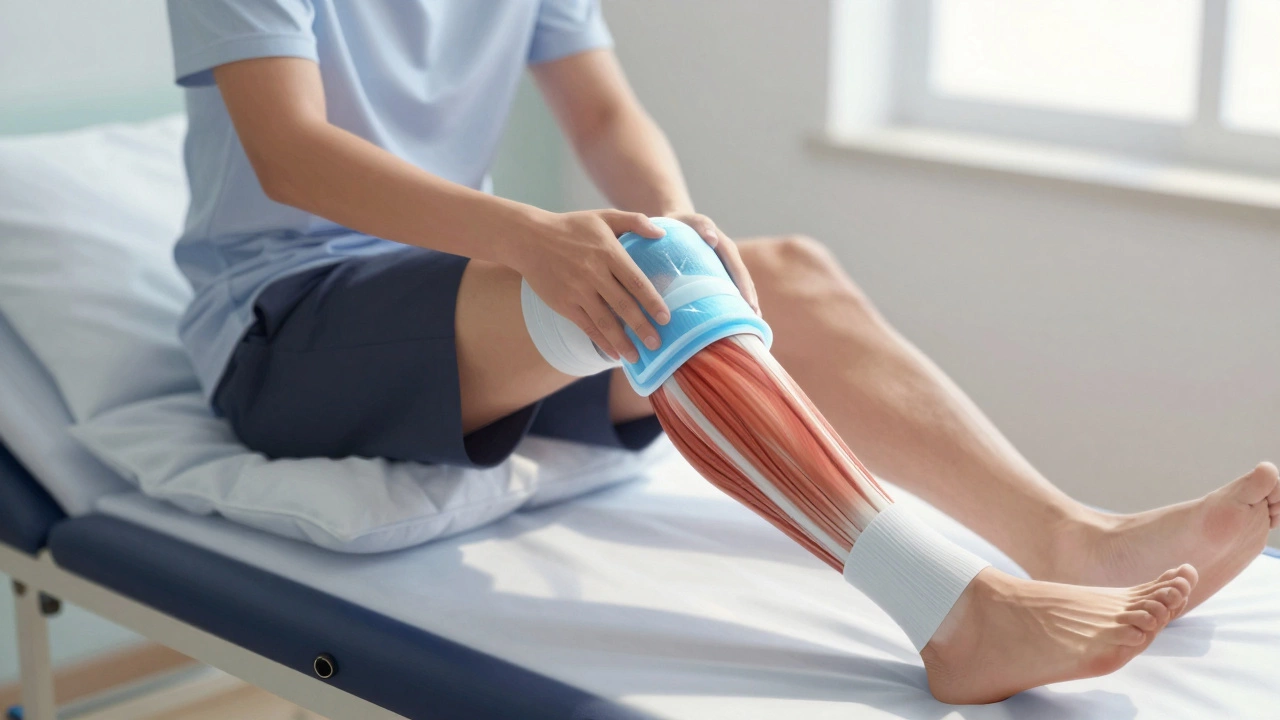
The Role of Swelling in Persistent Pain
Swelling is the silent culprit behind prolonged discomfort. Even after the initial surgical pain fades, many patients report that their knee feels "full" or tight for months. This is due to residual edema in the soft tissues. Gravity plays a major role here. If you keep your foot flat on the floor for too long, fluid pools in the knee, increasing pressure and pain.
Elevation is not optional; it is essential. To be effective, your foot must be higher than your heart. Propping your leg up on pillows while lying down promotes venous return and lymphatic drainage, reducing the volume of fluid in the joint. Compression stockings also help by applying external pressure to prevent fluid accumulation in the lower leg.
If swelling persists beyond the first few weeks despite elevation, it may indicate overactivity. Doing too much too soon can reignite inflammation. Listen to your body. If your knee swells noticeably after physical therapy, reduce the intensity of your exercises the next day. Balance is crucial.
Nerve Pain and Sensory Changes
Some patients experience unusual sensations like tingling, numbness, or burning skin around the incision. This is known as neuropathic pain. During surgery, small sensory nerves are inevitably cut or stretched. As these nerves heal and regenerate, they send erratic signals to the brain.
This type of pain doesn't respond well to standard opioids. Instead, medications like gabapentin or pregabalin are often prescribed to calm nerve activity. Desensitization techniques can also help. Gently rubbing different textures (cotton, silk, wool) over the numb areas can retrain your brain to interpret these sensations as normal touch rather than pain.
It is important to note that some degree of numbness below the kneecap is permanent and normal. The saphenous nerve branch is often affected, leading to a patch of skin that never fully regains sensation. While this isn't painful, it can be unsettling. Be careful when checking water temperature or walking on hot surfaces to avoid burns since you won't feel the heat.
Managing Pain Without Over-Medicating
Relying exclusively on strong painkillers carries risks, including constipation, drowsiness, and dependency. A multimodal approach works best. This means combining different types of interventions to target pain from multiple angles.
- Ice Therapy: Apply ice packs for 20 minutes every hour while awake during the first week. Cold constricts blood vessels, reducing swelling and numbing the area.
- Medication Rotation: Alternate between acetaminophen and non-steroidal anti-inflammatory drugs (NSAIDs) if approved by your doctor. This maintains steady pain relief without exceeding safe dosage limits for either drug.
- Mental Distraction: Anxiety amplifies pain perception. Engaging in light activities like watching movies, listening to podcasts, or talking with family can shift your focus away from the discomfort.
- Breathing Techniques: Deep diaphragmatic breathing activates the parasympathetic nervous system, lowering stress hormones and reducing muscle tension.
Many patients underestimate the power of sleep. Poor sleep lowers your pain threshold, making everything hurt more the next day. Prioritize rest. Use pillows to support your legs in a comfortable position. If pain prevents sleep, take your prescribed medication 30 minutes before bed.
When Pain Signals a Problem
Not all pain is part of the normal healing process. Certain symptoms require immediate medical attention. Distinguishing between expected discomfort and warning signs is vital for avoiding complications.
Contact your surgeon immediately if you experience:
- Severe, unrelenting pain that does not improve with medication or rest.
- Redness, warmth, or pus draining from the incision, indicating infection.
- Sudden swelling in one calf accompanied by pain, which could signal a deep vein thrombosis (DVT).
- Fever above 101°F (38.3°C), suggesting systemic infection.
- Inability to bear weight or move the knee at all, which might indicate mechanical failure or dislocation.
Early detection of issues like infection or blood clots drastically improves outcomes. Don't hesitate to call your healthcare provider. It is better to be cautious than to risk serious complications.
The Long-Term Perspective
Recovery from knee replacement is a marathon, not a sprint. While the most intense pain subsides within the first two weeks, mild discomfort can linger for six months or more. This is especially true during weather changes or after periods of increased activity.
Most patients find that by three months, they are back to daily activities with minimal pain. The goal is functional improvement, not perfect sensation. Your knee may never feel exactly like a natural one, but it should allow you to walk, climb stairs, and enjoy life without the debilitating agony of osteoarthritis.
Patience and consistency in physical therapy are your greatest allies. Every small gain in range of motion and strength reduces strain on the joint, leading to less pain over time. Trust the process, follow your care team's advice, and celebrate each milestone, no matter how small.
How long does severe pain last after knee replacement?
Severe pain typically lasts for the first 3 to 7 days. After this period, pain transitions to a manageable ache or soreness. Most patients transition from strong prescription opioids to over-the-counter pain relievers within the first two weeks.
Is it normal to feel burning sensations around the incision?
Yes, burning or tingling sensations are common due to nerve regeneration and irritation. This usually improves over several weeks to months. If the burning is intense or accompanied by redness, consult your doctor to rule out infection or complex regional pain syndrome.
Why does my knee hurt more at night?
Nighttime pain can result from inflammation building up during the day, lack of distraction, or improper positioning. Elevating your leg above heart level and taking pain medication before bed can help. Anxiety and stress also heighten pain perception at night.
Can I use heat instead of ice after surgery?
Ice is generally recommended for the first few weeks to reduce swelling and numb pain. Heat can increase blood flow and swelling initially. Once acute swelling has subsided (usually after 2-3 weeks), heat may be used to relax muscles, but always check with your surgeon first.
What should I do if my pain suddenly gets worse after improving?
Sudden worsening of pain could indicate a complication such as infection, blood clot, or implant issue. Contact your orthopedic surgeon immediately. Do not ignore this symptom, especially if accompanied by fever, swelling, or redness.